Medical professionals talk heat stroke, Zika and snakebites
Story and photos by Amanda Eggert EBS Staff Writer
BIG SKY – Dr. Timothy Erickson peppered his Feb. 12 presentation on snake envenomation at Big Sky Resort’s Huntley Lodge with snake-related trivia, tossing out rubber snakes for correct answers.
At the Wilderness Medicine Conference, held Feb. 10-14, the audience refuses to be stumped, especially when Erickson, a National Geographic Explorers Club member, ups the ante and starts distributing microbrews, which he graciously opens.
They know which snake kills the most people worldwide – Russell’s viper. They know physical characteristics of venomous snakes of North America: arrow-shaped heads, heat-sensing pits between eyes and nostrils, and elliptical, cat-like eyes. They even know which state has the most snakebites per capita – North Carolina.
Erickson parts with 20-plus snakes during his 50-minute presentation. He also polls the crowd. About half the audience’s hands go up when he asks if anyone went skiing earlier in the day. Some are still wearing snow pants, vests and beanies.
“That was a heaven-kissed day, wasn’t it,” he says. “… All that sunshine, hardly any wind, a little powder in the morning?”
Approximately 400 people traveled from all over the U.S. as well as Canada, Australia and New Zealand to attend the National Conference on Wilderness Medicine, but it’s not all work. There are breaks built into each day for optional outdoor activities – think guided backcountry skiing, ice climbing and snowmobiling in Yellowstone National Park. Back indoors, attendees learn about topics like Zika virus and other mosquito-borne diseases, altitude illness prevention and treatment, and fracture and dislocation management in the backcountry.
Halfway through his presentation, Erickson asks if anyone’s been bitten by a snake. One hand goes up.
“Timber rattler,” she says.
“Where were you?”
“Tennessee.”
“Were you at a worship service?” Erickson quips, to appreciative laughter.
As the woman walks up to accept her Moose Drool Brown Ale from Erickson, she says, “I know you.” The two figure out they worked together in Antarctica years before.
He calls her in for a hug and says, “I am just so touched. Jenny, it’s just so wonderful to see you.”
———
When Dr. Eric Weiss co-founded the Wilderness Medicine program 25 years ago, he aimed to create a platform for medical education specific to wilderness and international settings.
“Before I went to medical school, I was a commercial raft guide. I used to see a lot of injured people in the wilderness and didn’t know how to take care of them,” he says. “After medical school [this] was a way for me to combine my passion with my profession.”
Weiss, now the course director, delivered a number of the conference’s lectures himself, including one titled “1001 Uses for Duct Tape & Safety Pins: Improvised Care in Austere Environments,” as well as others addressing medical issues related to temperature extremes. He’s a mountaineer, whitewater enthusiast and a professor of emergency medicine at the Stanford University Medical Center.
Attendees come from a broad range of medical backgrounds. Wilderness Medicine faculty have taught EMTs, search and rescue volunteers, psychiatrists, physicians from every specialty, radiologists, and physician assistants along with nurses; even Secret Service and military personnel.
“People love it,” Weiss said. “They’re learning about things they never learned in medical school and it’s info that’s vastly useful because it deals with stuff from day-to-day living.”
——
The conference, held at Big Sky for the past 21 years, is a mix of large lectures and optional smaller workshops that address the nuts and bolts of specific medical and backcountry skills.
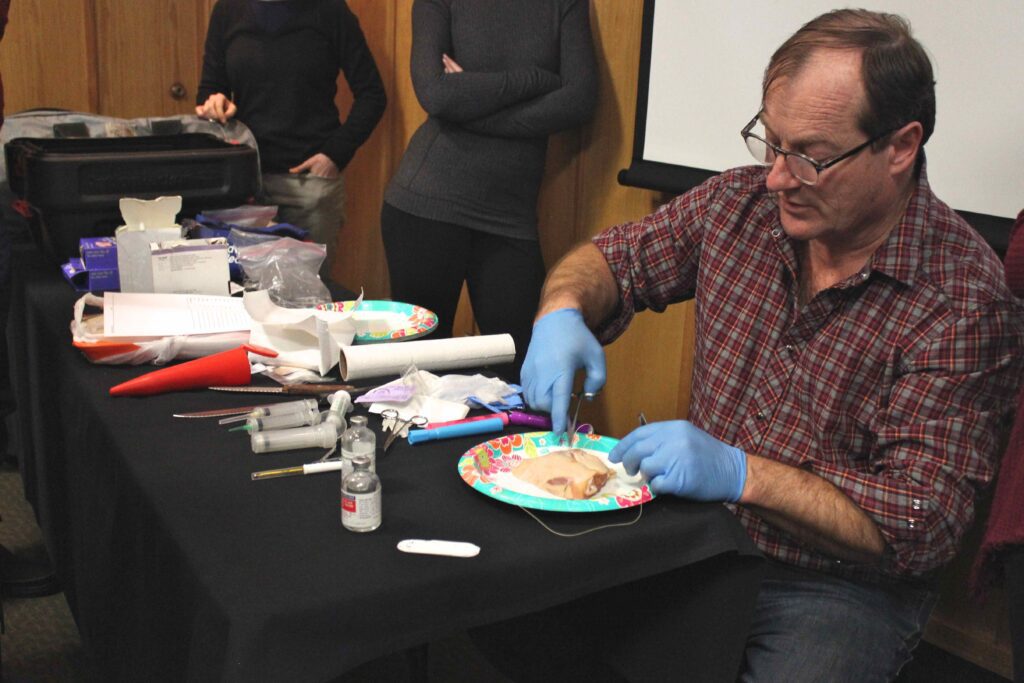
Physician Assistant Lanny Johnson led one such workshop, a suture lab and basic wound-management class, where about a dozen people practiced stitching up chicken breasts.
Johnson opened the workshop by stressing that it’s often best not to close wounds in the backcountry due to the difficulty in adequately cleaning them.
“There are almost no wounds that absolutely have to be closed, particularly on a backcountry expedition, even on a long expedition,” he said, adding that all backcountry wounds should be considered contaminated.
Sea wounds and snow wounds are no exception. “Don’t be fooled by snow. Snow is absolutely unclean. I’ve seen some of the worst pussed-out wounds from snow rash,” said Johnson, who serves as a medical advisor to the Jackson Hole Mountain Resort Ski Patrol.
Much of Johnson’s workshop is oriented toward the kind of wisdom-via-improvisation you might expect from a former climbing park ranger who is also a pilot: Always bring a headlamp with extra batteries, he says, but if you’re in a pinch you can use tinfoil to reflect light to better see inside a wound as you repair it.
Another tip: T-shirts boiled in water for 10 minutes will work if you don’t have sterile dressing available. Cover them with dry dressing and change them every one to three days.
“Every time you pull [the packing] out, that’s when [your patients] don’t like you,” he says in an almost offhand manner. “They’re going to hurt for a minute and you’re going to repack it.”
When it’s time to demonstrate different kinds of sutures, Johnson handles his instruments with ease and emphasizes the importance of stitching together similar tissue types: “‘Fascia to fascia, fat to fat. God doesn’t like people who don’t do that.’ When you sew, you have to recognize what you’re sewing together.”
After practicing running stiches and discussing the pros and cons of absorbable and non-absorbable sutures, Johnson’s workshop participants clean up.
He shares a couple more war stories, tells them to buy some chicken breasts to continue practicing, and leaves them with a final piece of advice: “If you feel like a goofball when you do this, don’t worry. It’s normal, totally normal.”













